Supraventricular tachycardia (SVT): quick, practical answers
Supraventricular tachycardia — usually called SVT — is a fast heart rhythm that starts above the heart’s ventricles. It can come on suddenly and make your heart race at 150–250 beats per minute. Most episodes aren’t life-threatening, but they can feel scary and sometimes need urgent treatment.
What SVT feels like and when to act
Typical signs are sudden palpitations, a pounding or fluttering chest, lightheadedness, shortness of breath, or sweating. Some people feel faint or have chest pain. If you get faint, have severe chest pain, are very short of breath, or feel weak and confused, call emergency services right away — those are red flags.
If the symptoms are milder — fast heartbeat but you’re stable — try to stay calm and sit down. Time the episode: tell your clinician how long it lasted and what you were doing when it started. That helps diagnosis.
What causes SVT and how providers find it
Common triggers include caffeine, alcohol, nicotine, certain cold medicines, dehydration, and big stress or lack of sleep. Underlying conditions such as thyroid problems or structural heart issues (including Wolff-Parkinson-White syndrome) can also cause SVT.
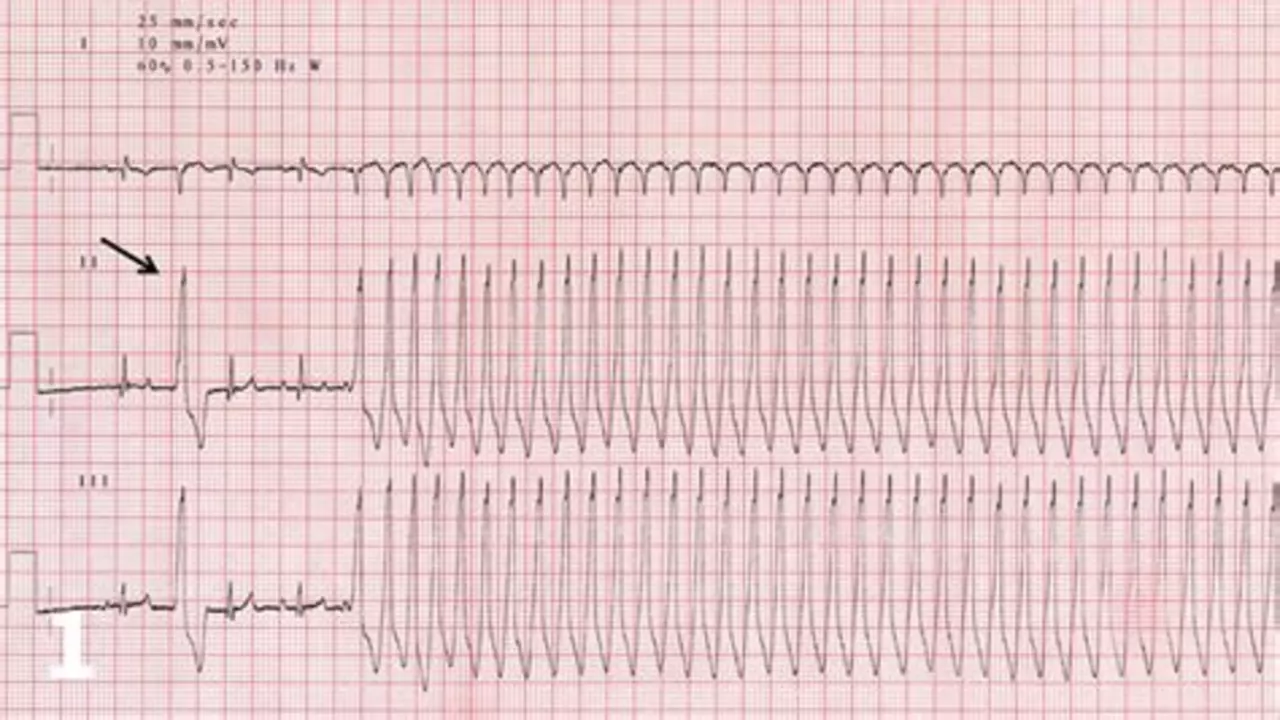
Doctors usually start with an ECG (electrocardiogram). If the ECG is normal between attacks, they might use a Holter monitor or an event recorder to catch an episode. An electrophysiology study (EPS) is an option when diagnosis or ablation is being considered.
Quick treatments and prevention tips
At home, simple vagal maneuvers can stop some episodes. Try bearing down like when you’re having a bowel movement (Valsalva maneuver) or splashing cold water on your face to trigger the diving reflex. Carotid sinus massage can work but only under medical supervision — do not try it if you have carotid artery disease.
In the clinic or ER, providers may give IV adenosine to slow the AV node and break the rhythm. If you’re unstable (very low blood pressure, chest pain, fainting), synchronized cardioversion is used right away.
For long-term control, options include beta-blockers, calcium channel blockers, or other antiarrhythmic drugs. The most definitive fix is catheter ablation — a minimally invasive procedure that targets the tissue causing the fast rhythm. Ablation often works well and can stop recurrent SVT.
Practical prevention: cut back on caffeine and stimulants, stay hydrated, manage stress, treat infections and thyroid problems, and talk to your doctor about medicines if episodes happen often. If your episodes are frequent or affect your life, ask about referral to an electrophysiologist to discuss monitoring and ablation.
Have questions about a specific medicine or test? Bring notes on what you felt, how long it lasted, and any triggers you noticed. That makes clinic visits far more useful and speeds up the right care for you.
Supraventricular Tachycardia in Athletes: Risks, Symptoms, and Management
Supraventricular Tachycardia (SVT) is a heart condition that can pose serious risks to athletes, causing symptoms like heart palpitations, dizziness, and shortness of breath. Although it's not common, when it does strike, it can seriously affect an athlete's performance and overall health. It's crucial to identify the symptoms early and manage them effectively to prevent complications. As an athlete, it's important to communicate any unusual symptoms to your healthcare provider for prompt diagnosis and treatment. Research and learning about SVT can also help athletes better understand and manage this condition.